Video
Consultation

عربى

Video
Consultation

Book An
Appointment

Accident & Emergency
99616 30000
Help Desk
99616 40000

Robotic
Surgery

Patients Login Portal
Best Cardiothoracic Treatment In Kochi.
Our experts treat babies and children with all types of congenital heart defects, including:

Mathrubhumi Arogyamasika cover story feature written by Dr. Abi Abraham M Director - Nephrology and Chief of Renal Transplant Services

കുരുന്നുകൾക്ക് ആകാശ സ്വപ്നം സഫലമായി

അമ്മമാർക്ക് സൗജന്യ ആരോഗ്യ പദ്ധതിയുമായി ലേക്ഷോർ

Endo robotic surgery performed on 75-year-old for oesophageal cancer
കൊച്ചി/മരട്, ജനുവരി 2, 2024 : പുതുവർഷത്തോടനുബന്ധിച്ചു വിപിഎസ് ലേക്ഷോറിൽ പ്രത്യേക ആരോഗ്യ പരിശോധന പാക്കേജുകൾ തുടങ്ങി.
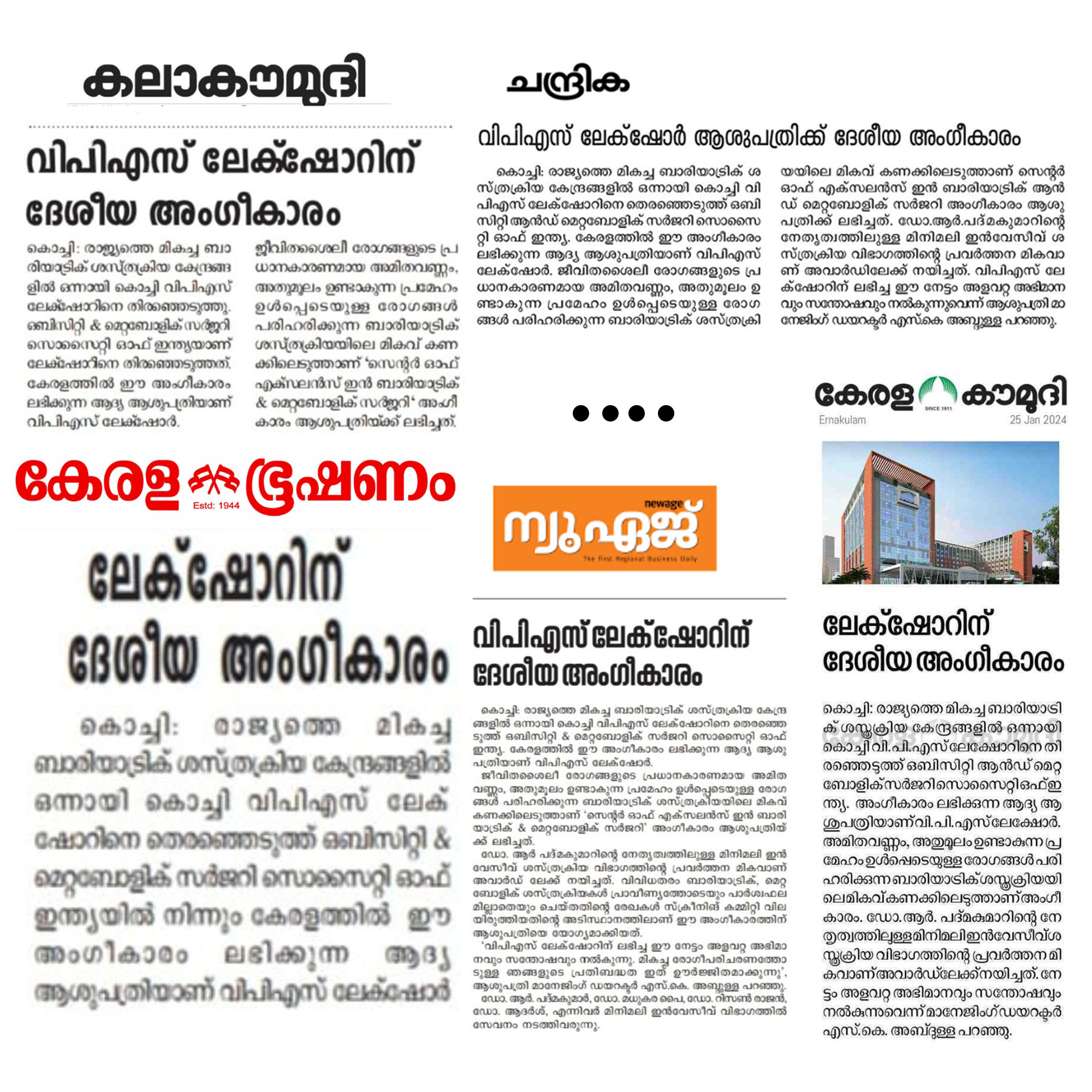
കൊച്ചി: രാജ്യത്തെ മികച്ച ബാരിയാട്രിക് ശസ്ത്രക്രിയ കേന്ദ്രങ്ങളിൽ ഒന്നായി കൊച്ചി വിപിഎസ് ലേക്ഷോറിനെ...
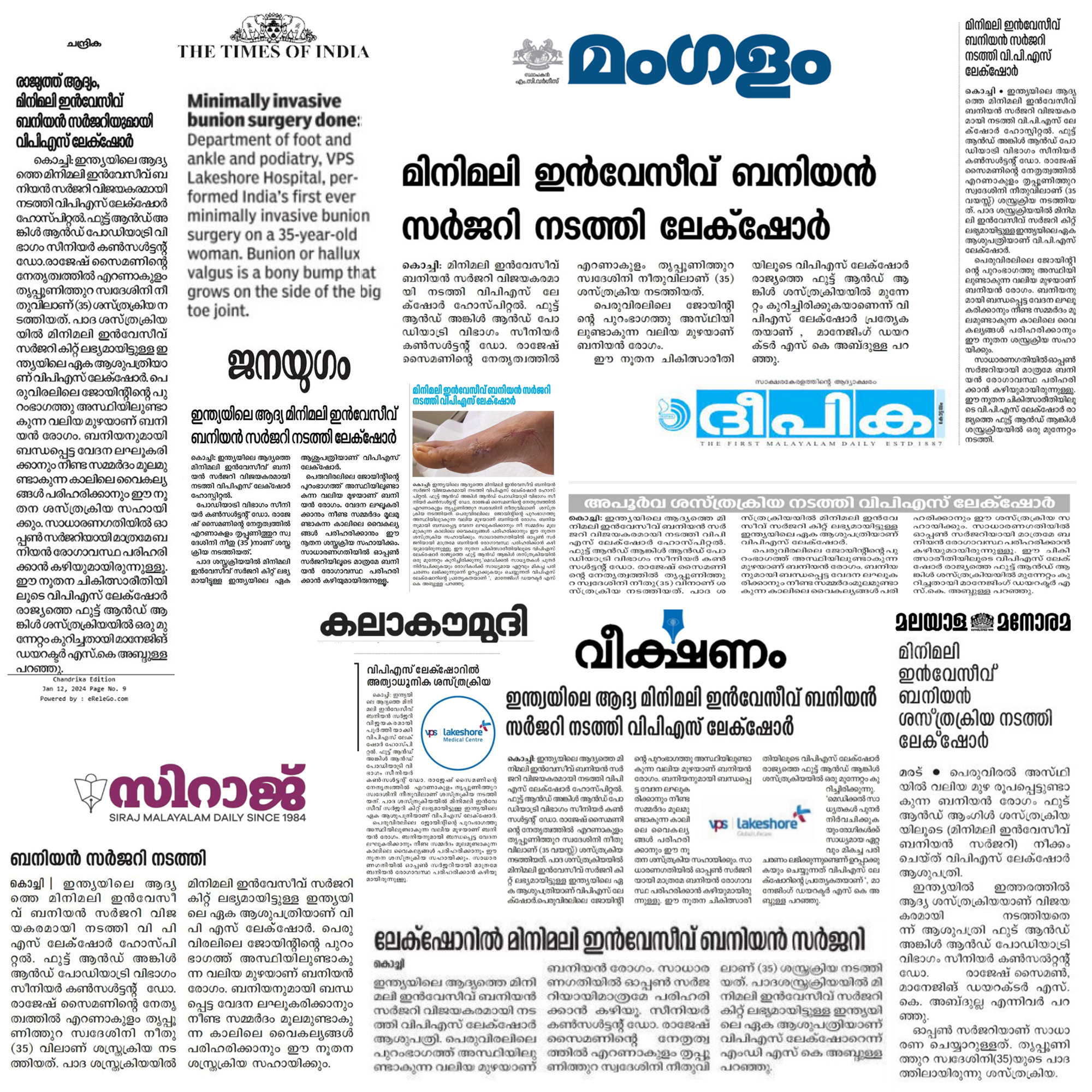
കൊച്ചി, 10 ജനുവരി 2024: ഇന്ത്യയിലെ ആദ്യത്തെ മിനിമലി ഇൻവേസീവ് ബനിയൻ സർജറി.....

കൊച്ചി, 16 ജനുവരി 2024 40% ഇളവിൽ ഗ്യാസ്ട്രോ പാക്കേജുകളുമായി വിപിഎസ് ലേക് ഷോർ. 9480 രൂപയുടെ...